High-risk Prostate Cancer Watershed: HRD Score + IDC-P Precise Stratification: An Overview
Intraductal prostate cancer (IDC - P) represents a subtype of prostate cancer characterized by a poor prognosis. Prior research has suggested that IDC - P may possess a potentially unstable genome. Homologous recombination defect (HRD) scoring is an outcome - based approach employed to depict genomic instability states. This article will investigate the correlation between the HRD score and IDC - P, along with other clinicopathological factors, as well as the prognostic impact of the HRD score within the cohort of aggressive prostate cancer.
Part 1 Background
Genomic instability is a characteristic trait of cancer. Homologous recombination defects (HRD) exert a significant influence on genome instability and can be targeted by poly ((ADP - ribose) polymerase inhibitors (PARPis)).
The therapeutic effectiveness of PARPis in ovarian cancer, breast cancer, pancreatic cancer, and prostate cancer (PCa) has been acknowledged. However, current testing methods are insufficient for identifying all patients who are sensitive to PARPi. Although HRD is a valid treatment target, there are still uncertainties regarding the precise definition of HRD.
Approximately 20% of PCa patients exhibit DNA damage repair (DDR) gene defects and may present with more aggressive disease characteristics [1].
Although germline DDR genes, especially BRCA mutations, are still considered as clinical predictors for PARPi use, DDR mutations are not adequate to comprehensively characterize the patient's HRD status.
Moreover, there are some inherent limitations in the genomic detection of DDR mutations: reversion mutations, epigenetic regulation, and potential predictive mutations of other genes. Particularly in PCa, the double - allele effect is more prominent when it is solely caused by somatic gene deletion [2].
However, the detailed distribution of HRD scores in prostate cancer (PCa) remains unclear. Current comprehensive studies have produced conflicting results regarding PCa [3]. A thorough understanding of HRD scores in PCa will enable more effective stratification of patients for HRD - targeted therapies.
In addition, PCa exhibits heterogeneity in pathological subtypes, and these aspects seem to be inadequately researched. Related research reports have documented the prognostic and molecular differences among different PCa pathological subtypes [4]. It is noteworthy that, aside from being associated with unfavorable clinicopathological characteristics and poor prognosis, intraductal prostate cancer (IDC - P) differs from adenocarcinoma (AC) in terms of genomic and transcriptomic features. Previous studies have indicated that the proportion of genomic abnormalities in IDC - P is higher [5]. Therefore, it is hypothesized that the genomic scarring of tumors potentially containing IDC - P components increases, resulting in a higher HRD score.
Researchers at the West China Hospital of Sichuan University conducted a study on 123 PCa patients, including those with high - risk localized (M0) and newly - diagnosed metastatic (M1) disease. The association of the HRD score with IDC - P and other clinicopathological factors, as well as the prognostic impact of the HRD score in the cohort of aggressive prostate cancer, was investigated. This HRD score is calculated based on over 10,000 single - nucleotide polymorphisms distributed across the human genome.
Using the rank - sum test, Chi - square test, Kaplan - Meier curve, and Cox proportional - hazards method, the researchers explored the association between the HRD score and clinicopathological characteristics, genomic alterations, and patient prognosis. To assess genomic scarring, the 3DMed - HRD algorithm [6] was developed based on over 10,000 single - nucleotide polymorphisms distributed in the human genome [6]. These polymorphisms are also included in the 156 and 733 gene next - generation sequencing (NGS) assays. The identification of homologous recombination repair (HRR) pathway genes is based on previous studies. All mutations in this study refer to deleterious or suspected deleterious mutations.
The median homologous recombination deficiency (HRD) score of this cohort was 21.0. Among these patients, 65 (52.8%) had an HRD score of 21 or greater. The HRD score of invasive ductal carcinoma - papillary (IDC - P) tumors is higher than that of adenocarcinomas. Other factors associated with high HRD scores include high M1 and International Society of Urological Pathology (ISUP) scores (4 - 5). MYC mutations were correlated with high HRD scores in the overall cohort. TP53 mutations and homologous recombination repair (HRR) pathway mutations corresponded to high HRD scores in IDC - P - positive patients and non - IDC - P patients, respectively, and the inverse relationship also held. An HRD score higher than 21 indicates that the overall cohort has a significantly poor survival rate. A high HRD score (≥21) is associated with a shorter cancer - free survival (CFS) period (ranging from 22.6 months to 32.8 months, P = 0.004).
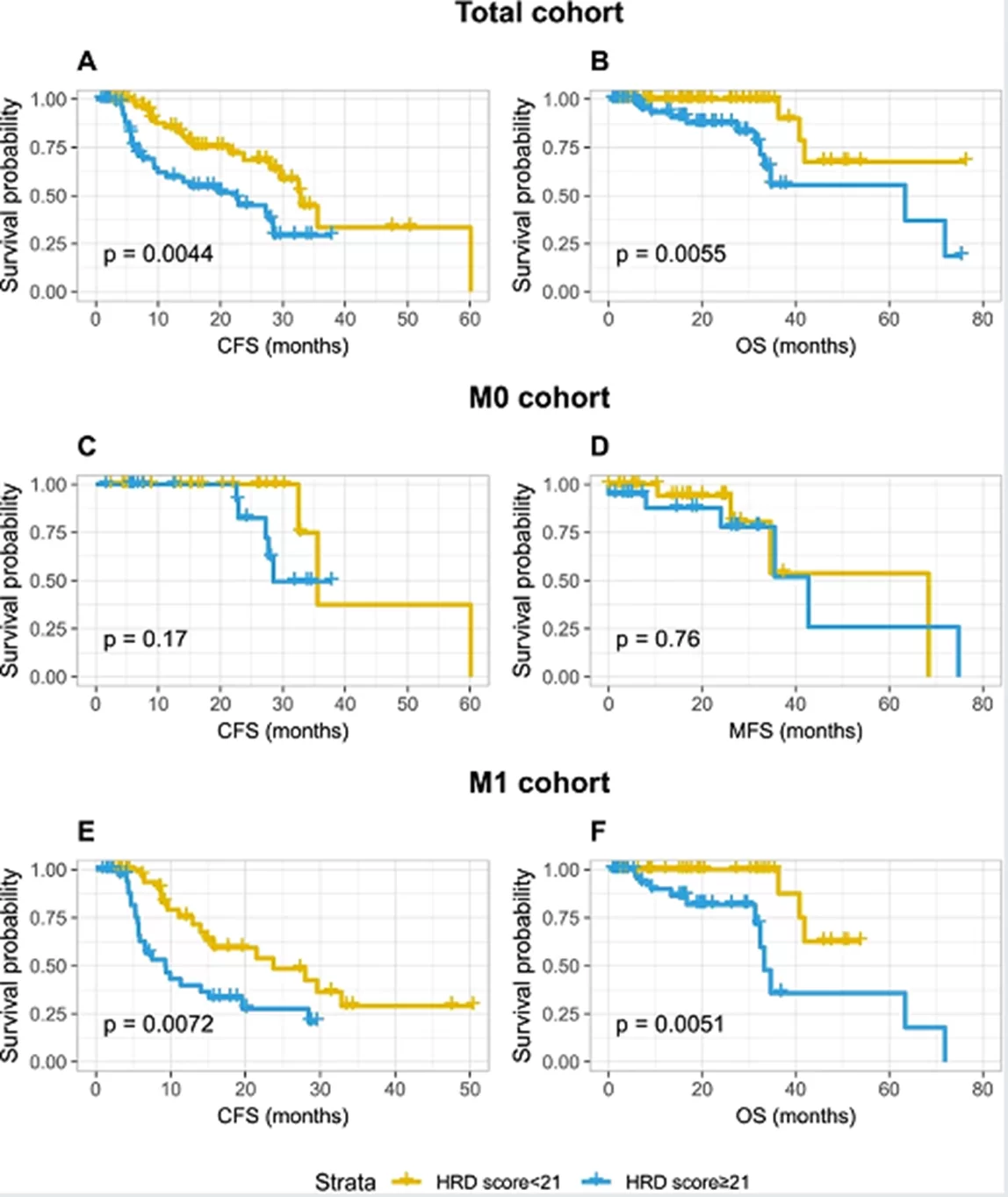
▲Prognostic value of HRD score
Part 2: Research Results
M1 stage, high ISUP scores, and IDC - P pathotyping may suggest higher HRD scores in prostate cancer (PCa). Tumor patients with IDC - P may have a distinct driving mechanism for high HRD scores compared to non - IDC - P patients. The HRD score demonstrates prognostic value within this positive cohort of prostate cancer.
Part 3: Summary
The study initially reported that patients with IDC - P components had significantly higher HRD scores than those with acinar carcinoma (AC). By utilizing a cohort that included both localized and metastatic patients, the researchers discovered that M1 patients were more prone to having higher HRD scores than M0 patients. Gene mutations beyond those in the homologous recombination repair (HRR) pathway (such as MYC and TP53) are also associated with higher HRD scores in PCa. Genetic alterations in the HRR pathway primarily drive the phenotype of high HRD scores in patients without IDC - P, while TP53 mutations only signify high HRD scores in patients with IDC - P. This disparity has not been previously observed and may hold important molecular significance.
In addition, patients with high HRD scores were found to have poorer survival rates in aggressive prostate cancer. High HRD scores in patients with IDC - P may be attributed to changes in TP53. This finding further emphasizes the possible heterogeneity of genomic maintenance mechanisms among different PCa pathological subtypes. Therefore, IDC - P may differ from AC in terms of the driving mutations of chromosomal instability.
Even if the homologous recombination (HR) function is restored, the existing genomic scars are unlikely to vanish. Therefore, it is strongly advised that high - risk patients undergo HRD testing at the early stages of the disease, and it is preferable to repeat the testing as the disease progresses. Patients with newly developed metastatic PCa, as well as those with IDC - P or high ISUP scores, have higher HRD scores. The HRD status of patients with IDC - P can be caused by abnormal factors outside the HRR pathway. It is recommended that patients with high - risk prostate cancer undergo HRD score testing, as this result can serve as a useful predictive and prognostic marker in aggressive prostate cancer.
References
[1] Cell. 2019;176(4):831–43. e22.
[2] Prostate. 2018;78(5):401–7.
[3] Nucleic Acids Res. 2004;32(Database issue):D493–6.
[4] Ann Oncol. 2020;31(4_suppl);S790.
[6] Br J Cancer. 2012;107(10):1776–82.
Statement: This article is only for sharing. If it involves copyright and other issues, please contact us as soon as possible and we will correct it as soon as possible. Thank you!





 闽公网安备35021202000745
闽公网安备35021202000745