Application of Molecular Classification in Guiding the Care and Treatment of Patients with Endometrial Cancer or Endomet
Application of Molecular Classification in Guiding the Care and Treatment of Patients with Endometrial Cancer or Endometrial Intraepithelial Neoplasia
Background of care and treatment
Endometrial cancer (EC) is one of the common malignant tumors of the female reproductive system. In 2016, there were 71,100 new cases of uterine cancer and 17,100 deaths in my country, the vast majority of which were EC. In recent years, the incidence of EC in my country has increased, and the incidence among young women is on the rise, especially in developed cities. Up to 14% of patients are women of childbearing age, who may have a good long - term prognosis and want to retain their fertility. With the changes in my country's fertility policy and the increase in the number of young women delaying childbirth, the proportion of these patients is increasing. Therefore, fertility - preserving treatment is an important appeal for these young women with EC [1].
According to the NCCN guidelines, the prerequisites for early treatment are as follows:
(1) Well - differentiated (G1) endometrial carcinoma (EEC) confirmed by a pathologist after diagnostic uterine scraping;
(2) Nuclear magnetic resonance imaging (MRI) or transvaginal ultrasound confirms that the lesion is limited to the endometrium;
(3) Imaging examination shows no other suspicious metastatic lesions;
(4) There are no contraindications to drug treatment or pregnancy;
(5) The patient must be informed that fertility - preserving treatment is not the standard treatment method of EC [2].
Treatment mainly uses progesterone - based continuous treatment: one can take Megestrol Acetate, Medroxyprogesterone Acetate Tablets, or use a Levonorgestrel intrauterine device (LNG - IUS) [3].
Molecular classification of endometrial cancer
The molecular classification of EC has been one of the hot topics in the field of gynecology in the past two years. In 2013, the Cancer Genome Atlas (TCGA) included 373 EC patients with different tumor stages, histological types, tumor differentiation levels, and adjuvant therapy methods. Multi - omics detection methods were used to divide EC into 4 subtypes based on mutation types and copy number differences, namely POLE super - mutant, Microsatellite instability (MSI) high - mutation type, low copy number (CN - L) type, and high copy number (CN - H) type. The study found that there are significant differences in the progression - free survival (PFS) of the four subtypes: the POLE mutant has the best prognosis, the CN - H type has the worst prognosis, and the MSI type and CN - L type are in the middle (P = 0.02) [4]. Subsequent studies such as ProMisE and TransPORTEC have all reached similar conclusions [5 - 6].
The TCGA study found that according to the mRNA sequencing results, there is an increase in the expression of progesterone receptor (PGR) in CN - L tumors, suggesting that this part of the patients may have a response to hormone therapy. Further analysis found that compared with the other three subtypes, the expression of PGR in the CN - L subtype increased, all with significant differences [4].
Research Progress Abroad
A South Korean study conducted an evaluation of 57 patients undergoing care treatment. The rate of complete remission (CR) or partial remission (PR) among patients with mismatch repair defect (MMRd) was significantly lower than that of p53 wild - type (p53wt) patients (44.4% vs 82.2%, P = 0.018). There were also significant differences in the CR rate (11.1% vs. 53.3%, P = 0.01) and the cumulative CR rate (p = 0.035) at the specified month. Among MMRd - type patients, 4 cases underwent immediate hysterectomy due to treatment failure, and 3 cases had a diagnosis upgrade following hysterectomy. The study concluded that molecular classification holds prognostic significance in the management of endometrial cancer (EC) fertility retention, and the MMR status can serve as a predictive biomarker to exclude patients who can benefit from hormone therapy [7].
Through immunohistochemistry (IHC) testing, American researchers discovered that 6 cases (7%) of patients with atypical endometrial hyperplasia or FIGO stage I endometrioid endometrial cancer (EEC) aged ≤55 years had MMR protein deficiency. These patients exhibited a higher incidence of invasive cancer and a poor response to progesterone therapy. The tumor regression rate of deficient mismatch repair (dMMR) patients was 0, which was significantly different from that of patients with normal mismatch repair function (pMMR) (p = 0.028). All 6 dMMR patients ultimately underwent surgery [8]. Another Italian study also found that dMMR patients were more commonly resistant to chemotherapy than pMMR patients (33.3% vs 15.9%), although this difference was not statistically significant (P = 0.2508). The recurrence rate of dMMR patients was significantly higher than that of pMMR patients (100% vs 26.4%, P < 0.0001), and the specificity of dMMR in predicting recurrence reached 100% [9].
Researchers such as Allison M. Puechl evaluated whether molecular classification can predict the response of patients with EC and endometrial intraepithelial neoplasia (EIN) to levonorgestrel - intrauterine system (LNG - IUS) treatment. According to ProMisE's classification strategy, it employs IHC to detect MMR and p53 proteins and sequencing to detect POLE exonuclease domains. The study enrolled 58 patients, among which 22 (37.9%) had EC and 36 (62.1%) were EIN; 44 (75.9%) were classified as p53wt type, 6 (10.3%) were classified as MMRd type, 4 (6.9%) were classified as p53 abnormal (p53abn) type, and 4 cases (6.9%) were classified as POLE mutant. Among the 11 cases (19.0%) that progressed (PD) or changed treatment methods, the p53abn type progressed the fastest [10].
The latest domestic research[1]
Recently, the Pathology Department/Obstetrics and Gynecology of Peking University People's Hospital cooperated with SpaceGen to use SpaceGen's molecular classification test for endometrial cancer to evaluate the relationship between molecular classification and the treatment response of women with EEC or atypical endometrial hyperplasia/endometrial intraepithelial neoplasia (EAH/EIN). The relevant research results were published in the journal PATHOL RES PRACTICE (IF = 3.309).

The researchers conducted a retrospective analysis of 39 EEC and 20 EAH/EIN patients who received reserved fertility treatment between 2013 and 2021. All patients were treated with high - dose progesterone (500 mg per day), with ultrasound monitoring once a month and hysteroscopy once a quarter. The researchers performed IHC analysis of biopsy samples, including p53 and MMR proteins (MSH2, MSH6, PSM2, MLH1), and used SpaceGen's self - developed molecular classification kit for endometrial cancer for molecular testing.
The median age of patients was 33.4 years old. The median follow - up period of the study was 16.8 months, during which 4 patients gave up progesterone treatment due to PD. 23 of the 39 EEC patients reached CR after intensive treatment, which was significantly lower than that of the EAH/EIN group (58.97% Vs. 80.0%, P < 0.05). The samples of 59 patients have completed molecular classification, and the distribution of the four subtypes is: 83.05% (49/59) are CN - L type, 6.78% (4/59) are MSI - H type, and 5.08% (3/59) are POLE super mutant and CN - H type. The MSI and TP53 sequencing results are consistent with the IHC analysis of MMR and p53 proteins. The proportion of patients with each molecular subtype reaching CR was: POLE super mutant type was 100% (3/3), CN - L type was 71.43% (35/49), MSI - H type was 25% (1/4), and CN - H type was 33.3% (1/3). The prognosis of POLE super mutant and CN - L types is better than that of MSI - H and CN - H types.
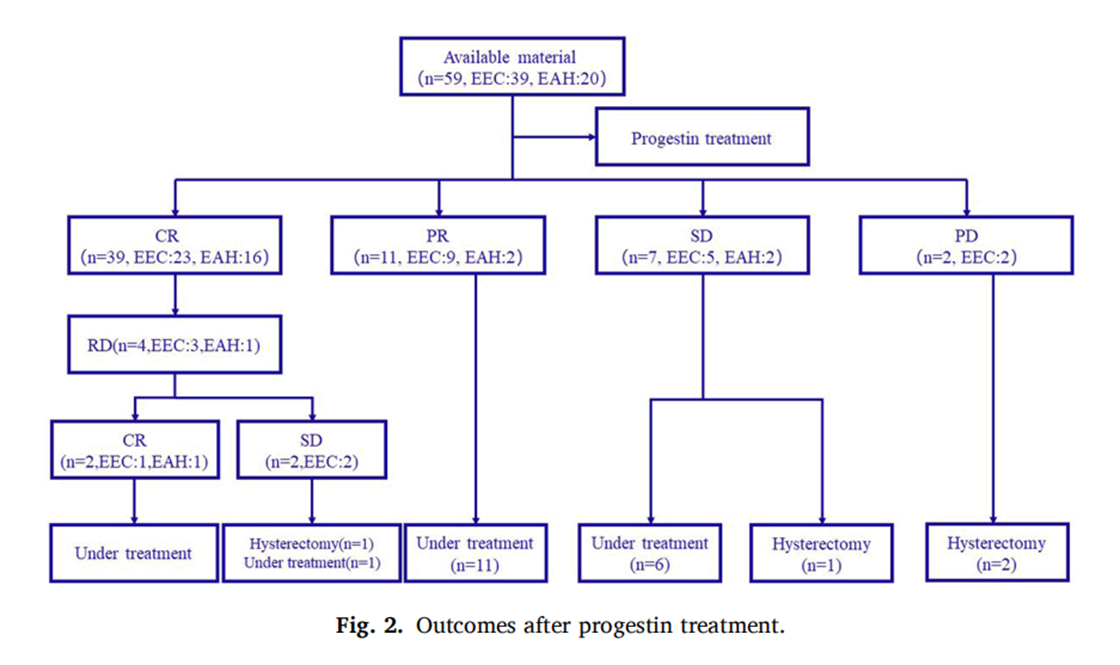
▲The outcome of progesterone treatment
This study is one of the first to report the relationship between molecular classification and the childcare outcome of EEC or EAH/EIN females, and it is also the first similar study based on the Chinese population. The molecular classification of EAH/EIN has rarely been reported before. This study included 20 cases of EAH/EIN, which met the requirements of quality control and obtained the classification results. More importantly, unlike previous researchers who focused on morphological changes, during treatment and follow - up, this study combined morphology and molecular testing to evaluate the relationship between molecular classification and prognosis.
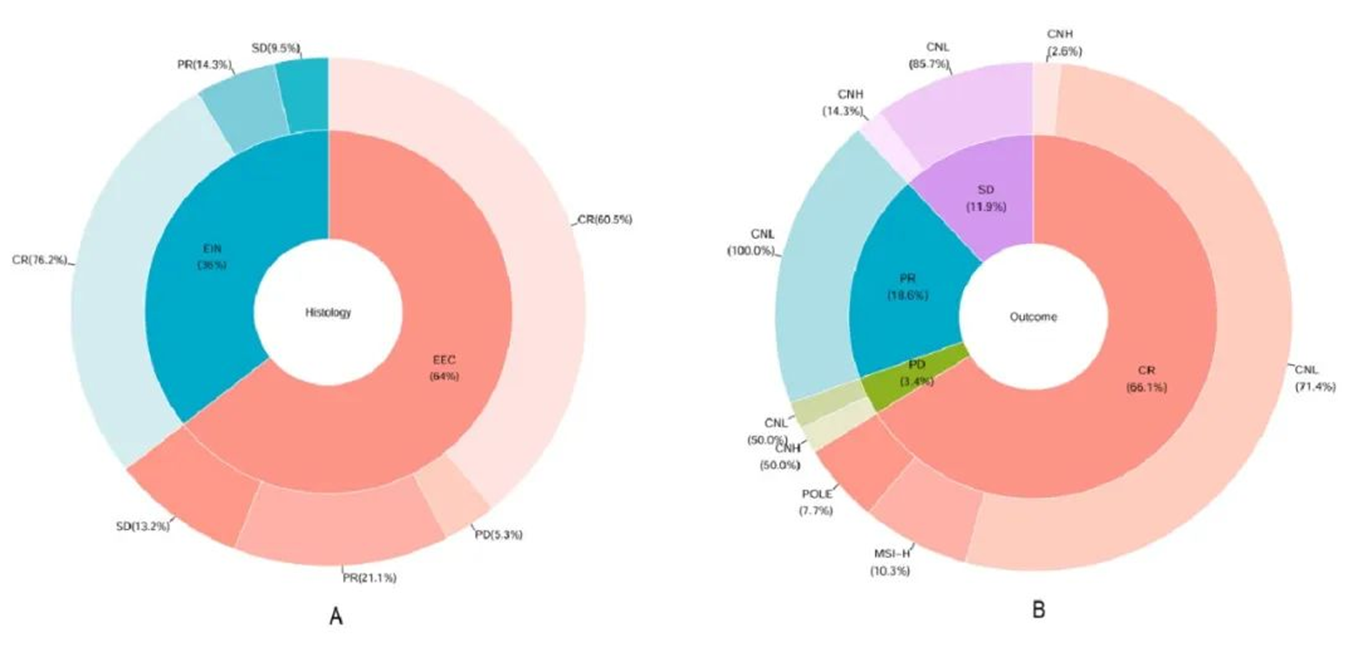
▲The outcome of patients with different histological types (A) and molecular subtypes (B)
Most of the samples in this study were CN - L type, which is related to the low - level EEC and EAH/EIN of these patients. The prognosis of MSI - H patients varied greatly, with one case each of CR, PR, recurrence (RD) and PD. This also confirms that MSI - H patients are less sensitive to hormone therapy than pMMR patients. CN - L and POLE mutants are more sensitive to gene therapy, which may be related to higher levels of PGR expression. CN - H type is not sensitive to hormone therapy and has a poor prognosis. Although EAH/EIN and low - level EEC are relatively inert, the results of this study show that TP53 mutations and MSI - H status may indicate poor treatment results.
Conclusion
Young patients with EAH/EIN or low - level EEC who wish to retain reproductive function can consider childcare treatment. Compared with EEC patients, EAH/EIN patients have better efficacy. It is feasible to perform molecular classification of EAH/EIN. Prior to progesterone therapy, the molecular classification of EEC and EAH/EIN biopsy samples may predict patients at risk of advancement[1].
Molecular classification of endometrial cancer by SpaceGen
SpaceGen's molecular classification of endometrial cancer uses high - throughput sequencing methods to comprehensively detect the classification markers and auxiliary classification factors recommended by the guidelines, which have suggestive effects on the prognosis, adjuvant therapy, immunotherapy, hormone therapy and genetic risk of EC patients. SpaceGen is committed to providing the most innovative products and services for personalized precision medical testing of tumors and continuously updating existing products.
References
[1] Pathol Res Pract. 2022 Dec 19;241:154278.
[2] NCCN Clinical Diagnosis and Treatment Guidelines for Uterine Tumors 2023 v1
[3] Guidelines for Diagnosis and treatment of Endometrial cancer (2021 Edition)
[4] Nature. 2013 May 2; 497(7447):67-73.
[5] Ann Oncol. 2018 May 1; 29(5): 1180-1188.
[6] J Clin Oncol. 2020 Oct 10; 38(29): 3388-3397.
[7] Am J Obstet Gynecol. 2021 Apr;224(4):370. e1-370. e13.
[8] BJOG. 2017 Sep;124(10):1576-1583.
[9] Gynecol Oncol. 2021 Jun;161(3):795-801.
[10] Cancers (Basel). 2021 Jun 7;13(11):2847.



 闽公网安备35021202000745
闽公网安备35021202000745