Exploration of the Prognosis of dMMR-Type Endometrial Cancer Complicated by TP53 Mutation
PART 1: What Is Endometrial Cancer with Multiple Molecular Characteristics?
The molecular classification of endometrial cancer has achieved global consensus. Among them, the TCGA typing system classifies it into four categories: POLE mutant, MSI - H (dMMR) type, p53 mutant (with multiple TP53 abnormalities), and the group without specific molecular modifications.
In clinical practice, most tumors exhibit only one molecular characteristic, yet approximately 3% - 11% of patients simultaneously carry two or more molecular characteristics. Such tumors are defined as "endometrial cancer with multiple molecular characteristics" [1,3].
Among all multi - classified tumors, the combination of dMMR and TP53 mutation (MMRd - p53abn) is the most prevalent type, accounting for approximately 6.6%, which is significantly higher than other combined types [1].
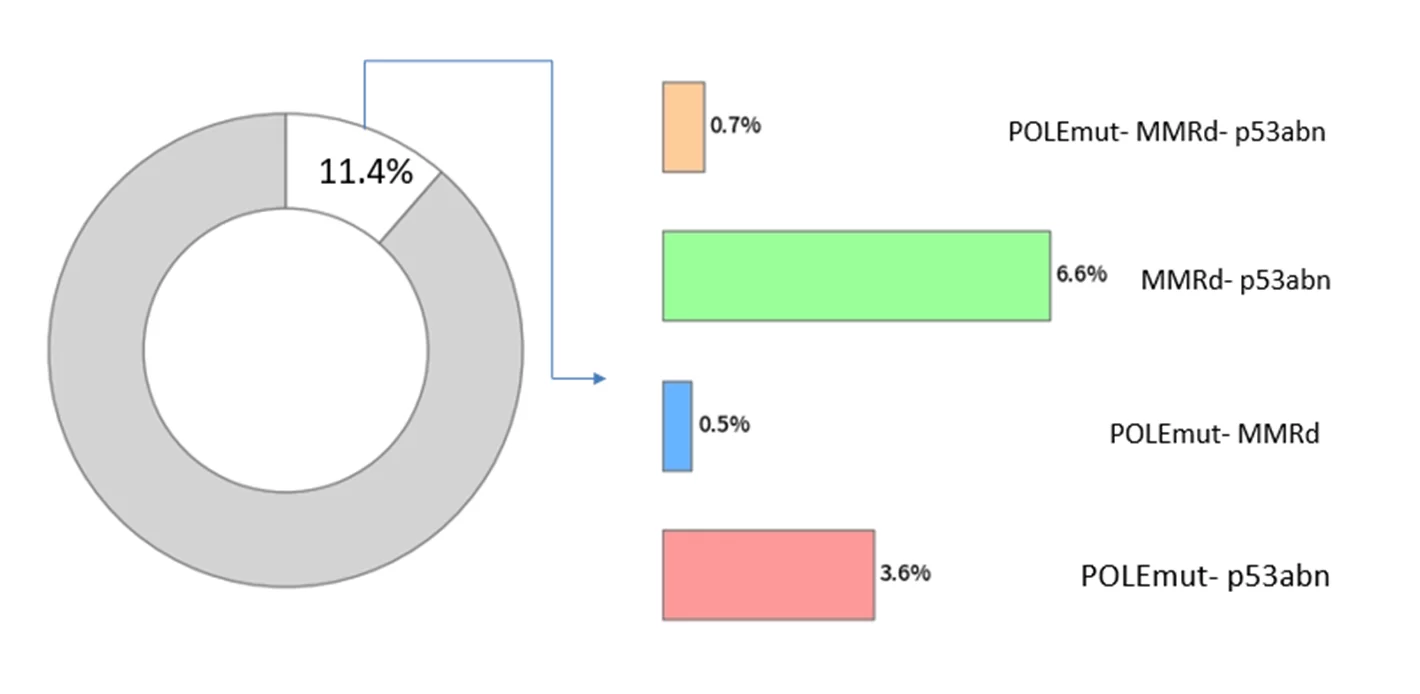
▲Figure 1. Multiple molecular characteristics, distribution, and proportion of endometrial cancer
The discovery of this type is attributed to comprehensive molecular detection technology. Only some cases might be overlooked through immunohistochemistry. When combined with next - generation sequencing (NGS) technology, this special typing can be captured more accurately.
In the past, there has been a clear clinical understanding of the prognostic judgment of single molecular characteristics:
Single TP53 abnormality (p53abn): A proper "bad prognostic signal". Research data indicate that the 5 - year recurrence risk of such patients is as high as 34.3%, and the 3 - year disease - free survival rate is only 38.0%. Most of them are advanced, non - endometrial carcinoma, which is highly aggressive [1].
Single dMMR(MSI - H): The prognosis is moderate to good. The 3 - year disease - free survival rate is approximately 91.9%, the recurrence rate is only 4.0%, and the response to immune checkpoint inhibitors is favorable [1].
When these two characteristics appear in a patient simultaneously, both the patient and the doctor are inevitably concerned: Will it be "worse"? How to judge the prognosis? Should the treatment plan be adjusted? These two seemingly "contradictory" molecular characteristics, one being often related to the benefits of immunotherapy and the other often indicating a poor prognosis, have put clinical judgment in a difficult position.
PART 2 Key Finding: The prognosis is in an "intermediate state", neither the worst nor the best
Based on the large - sample data of three major international clinical studies (including more than 4,000 patients with endometrial cancer in total), we have a clear answer to the prognosis of MMRd - p53abn patients: the prognosis of such patients presents unique "intermediate characteristics", which is significantly better than that of a single TP53 - abnormal patient, but slightly inferior to that of a single dMMR patient [1 - 3].
01. The risk of recurrence is significantly reduced, and the survival benefits are clear
Research data show that the recurrence rate of MMRd - p53abn patients is only 7.1%, which is much lower than the 23.3% of patients with a single TP53 abnormality; its three - year disease - free survival rate is as high as 87.8% (95% CI: 59.6 - 96.8), which is more than twice that of patients with a single TP53 abnormality (38.0%), p < 0.001 [1].
Another large - scale study involving 3,518 patients also confirmed that the 5 - year disease - free survival rate of MMRd - p53abn patients reached 83.4%, which was much higher than the 70.8% of patients with a single TP53 abnormality. The difference was statistically significant (p = 0.024) [3]. This data fully shows that the existence of dMMR characteristics significantly "neutralizes" the adverse prognostic effects of TP53 mutation.
02. The clinical features are milder and less invasive
Genetic testing combined with clinicopathological analysis found that most patients with MMRd - p53abn showed "low - invasive" clinical features [1]:
The staging is earlier: 60.7% are in stage I - II, and only 39.3% are in the advanced stage (stage III - IV), while the proportion of patients with a single TP53 abnormality in the advanced stage is as high as 53.4%;
The pathological type is better: 85.2% are endometrial carcinomas, and the proportion of non - endometrial carcinomas is only 14.8%, which is much lower than the 50.0% of patients with a single TP53 abnormality;
Malignant characteristics are rare: the incidence of diffuse lymphovascular gap infiltration is only 18.5%, and the rate of lymph node metastasis is 22.2%, which is lower than that of patients with a single TP53 abnormality.
These clinical features have laid the foundation for a good prognosis of MMRd - p53abn patients, and the accurate identification of these features is inseparable from the combination of genetic testing and pathological analysis.
03. TP53 mutation still has additional risks
There is still a gap compared with a single dMMR, and there is still an additional risk of TP53 mutation. It is worth noting that the prognosis of MMRd - p53abn patients is still slightly inferior to that of single dMMR patients [1]:
Recurrence rate: 7.1% vs 4.0%;
3 - year disease - free survival rate: 87.8% vs. 91.9%;
High - grade ratio: 55.6% is G3 grade, which is higher than the 22.2% of patients with single dMMR (p = 0.001).
This suggests that although TP53 mutation is not the dominant factor, it still poses a slight additional risk to the tumor. This detail can only be captured through precise molecular typing, and it also provides a basis for fine - tuning follow - up treatment options.
PART 3. Deep mechanism: TP53 mutation may be a "secondary mutation" here
Why are the "bad effects" of the TP53 mutation "neutralized" by dMMR? The molecular mechanism behind this can be revealed through NGS genetic testing technology [1,3].
1. The timing of the mutation is different, and TP53 is mostly a "secondary event".
The study found that in MMRd - p53abn tumors, TP53 variants are mostly expressed as "subclonal expression", which occurs in about 18.2% of patients, while only 2.9% of patients have a single TP53 abnormality (p = 0.005) [1].
Subclonal expression means that TP53 mutation is a "later" change in tumor progression, rather than the core factor driving tumor occurrence. In contrast, dMMR, as an earlier "driving event", has shaped the main biological behavior of tumors, which is also the key reason why dMMR can dominate the prognosis.
2. The molecular map is closer to dMMR than TP53.
Through the gene clustering analysis of tumor samples in the TCGA database, it was found that the single - nucleotide mutation (SNV) characteristics and copy - number change pattern of MMRd - p53abn tumors are closer to a single dMMR tumor (20/23 cases clustered in the dMMR group), rather than a single TP53 - abnormal tumor (only 3/23 cases clustered in the p53abn group) [3].
This molecular - level evidence further confirms that dMMR is the core feature that dominates the biological behavior of such tumors. TP53 mutations are more like "secondary mutations" and have not changed the essential properties of tumors.
3. The advantages of immune infiltration are retained to provide the basis for immunotherapy
The typical characteristics of dMMR tumors are high tumor mutation load (TMB) and rich immune infiltration, and this feature is preserved in MMRd - p53abn tumors [2,3].
The proportion of tumor - infiltrating lymphocytes (TILs) and lymphocytes is higher.
The positive rate of microsatellite instability (MSI) reached 92.3%.
Abnormal expression of MMR protein is mainly due to loss of MSH6 (55.6%), and such abnormalities are more likely to trigger an immune response.
This is also a key mechanism by which MMRd - p53abn patients can still benefit from immunotherapy.
PART 4 Clinical inspiration: Treatment Decision - making under the guidance of precise Genetic testing
The treatment decision for MMRd - p53abn patients should be based on accurate genetic test results to avoid "one size fits all" [1,2]:
1. To avoid over - treatment, refer to the principles of dMMR tumor treatment
Since dMMR is the dominant feature, MMRd - p53abn patients do not need to blindly strengthen treatment due to TP53 mutation:
Early - stage patients (Phase I - II): mainly undergo surgical treatment, combined with adjuvant radiotherapy (such as vaginal brachytherapy) if necessary, without conventional high - intensity chemotherapy;
Medium - and high - risk patients: adjuvant treatment options can be selected individually based on factors such as LVSI and muscle infiltration depth, and there is no need to upgrade to a combination of radiotherapy and chemotherapy due to TP53 mutation.
2. Immunotherapy can still be beneficial. For advanced patients, give priority to the molecular characteristics based on dMMR. MMRd - p53abn patients may still benefit from immune checkpoint inhibitor treatment [2]:
Patients with advanced or recurrent conditions: priority can be given to monotherapy with PD - 1/PD - L1 inhibitors, or combined with low - dose chemotherapy;
Clinical data support: The KEYNOTE - 158 study showed that the objective remission rate (ORR) of patients with dMMR/MSI - H endometrial cancer receiving treatment with pembrolizumab reached 46%, of which some patients were classified as MMRd - p53abn [2].
3. Emphasize comprehensive molecular testing to avoid missed diagnosis and misjudgment
Studies have confirmed that relying only on immunohistochemistry (IHC) may lead to missed diagnosis of some multi - classified tumors [1]:
TP53 sequencing can identify an additional 18.9% of MMRd - p53abn patients, and the p53 immunohistochemistry of these patients is normal;
Some MMRd - P53ABN patients have multifocal TP53 mutations (17.9%), and such complex variants cannot be identified by IHC alone.
References
[1] Int J Gynecol Cancer. 2024 Feb 5;34(2):229-238.
[2] Int J Mol Sci. 2024 Jan 15;25(2):1056.
[3] J Pathol. 2020 Mar;250(3):312-322.
Statement: This article is only for sharing. If it involves copyright and other issues, please contact us as soon as possible and we will correct it as soon as possible. Thank you!




 闽公网安备35021202000745
闽公网安备35021202000745