



DNA mismatch repair (MMR) is one of the DNA damage repair (DDR) mechanisms, and the key proteins involved in MMR function include MLH1, MSH2, MSH6, and PMS2. Mismatch repair deficiency (dMMR) refers to the loss of expression in at least one of these four MMR proteins, primarily caused by three mechanisms: germline mutations in MMR genes, somatic mutations, or methylation of the MLH1 gene promoter region. Compared to MMR gene mutations, MLH1 protein loss due to MLH1 methylation is more common. In colorectal cancer (CRC) and endometrial cancer (EC), abnormal MLH1 immunohistochemistry (IHC) results should prompt germline testing for MMR genes or MLH1 methylation analysis in tumor tissue, with methylation indicating sporadic tumors[1].
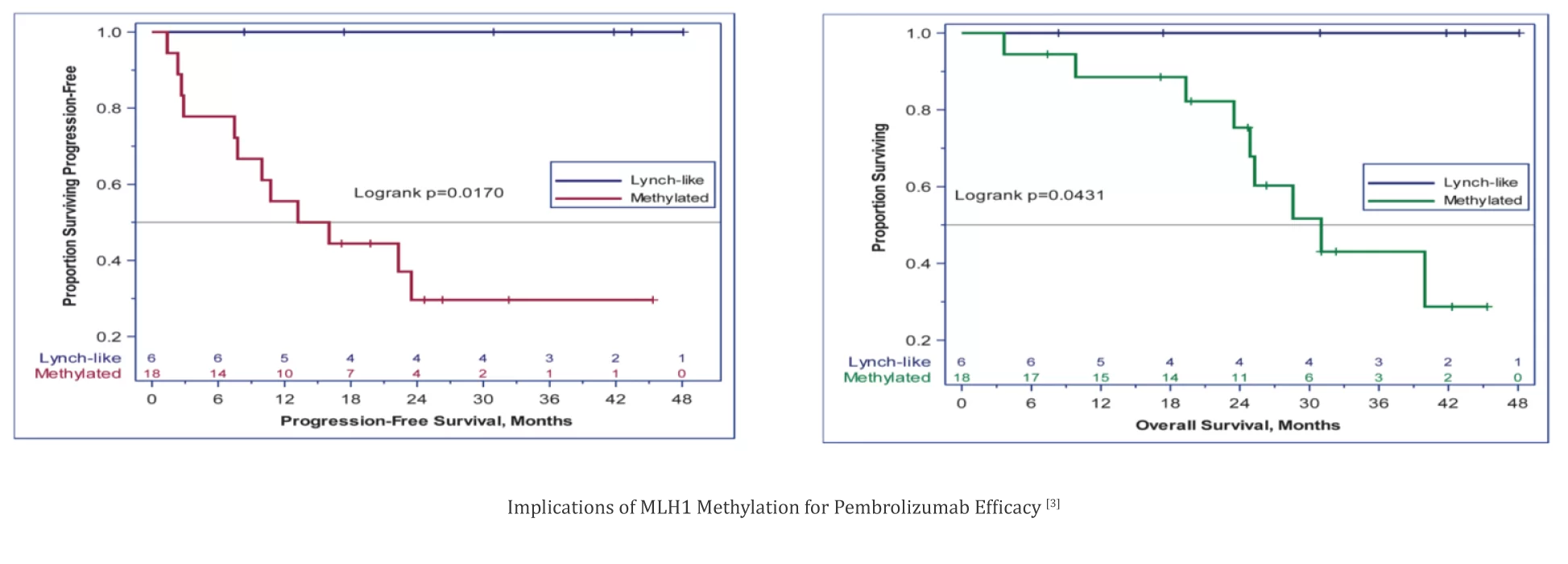
A Japanese study found that endometrial cancer with MLH1 promoter methylation had a significantly worse prognosis compared to suspected Lynch syndrome patients, with 5-year progression-free survival (PFS) of 95.2% vs. 78.1% (p=0.003) and 5-year overall survival (OS) of 94.6% vs. 79.2% (p=0.018) [2]. The Phase II trial (NCT02899793) evaluated Pembrolizumab in recurrent dMMR (deficient mismatch repair)/MSI-H (microsatellite instability-high) endometrial cancer, showing an objective response rate (ORR) of 100% in Lynch-like tumors versus 44% in sporadic tumors (p=0.024), 3-year PFS of 100% vs. 30% (p=0.017), and OS of 100% vs. 43% (p=0.043) [3].
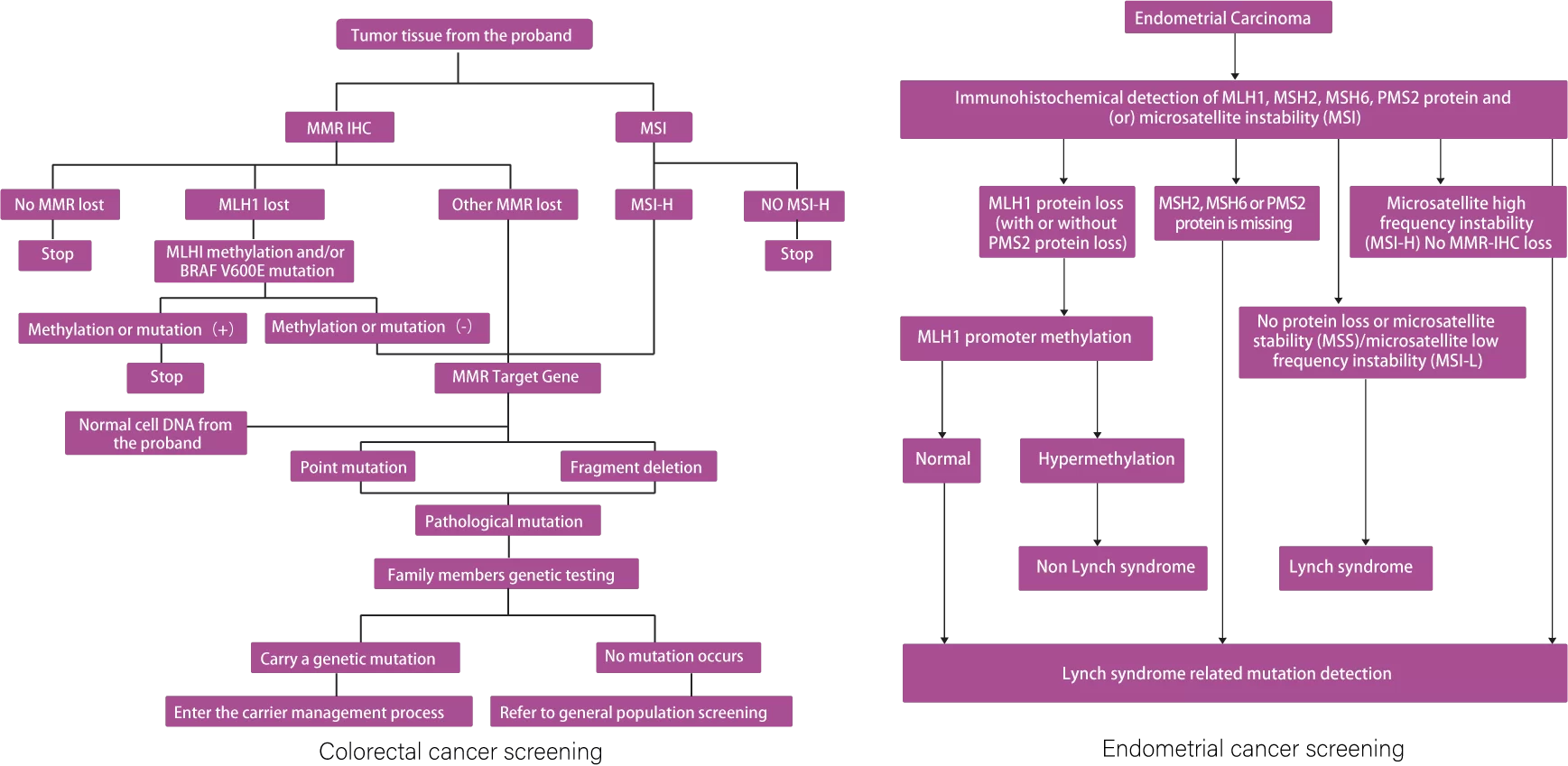
A study participated in by SpaceGen showed that discrepancies between MMR-IHC (mismatch repair immunohistochemistry) and MSI high-throughput sequencing (NGS) results frequently occur in cases with co-loss of MLH1 and PMS2 protein expression caused by hypermethylation of the MLH1 promoter or subclonal loss of MMR proteins. When necessary, detection methods such as MLH1 promoter methylation should be combined to comprehensively assess MMR and MSI status, providing accurate molecular profiling for endometrial cancer (EC) patients[4].
[1] NCCN Genetic/Familial High-Risk Assessment: Colorectal, Endometrial, and Gastric 2024 v3
[2] J Gynecol Oncol. 2021 Nov;32(6):e79.
[3] Cancer. 2022 Mar 15;128(6):1206-1218.
[4] DOI:10.3760/cma.j.cn112141-20230711-00316
333
1.Lynch syndrome screening MMR ( IHC ) found patients with MLH1 protein deletion ;
2.MSI-H colorectal cancer patients and endometrial carcinoma patients may consider detecting MLH1 gene methylation.
1. Indicates risk of Lynch syndrome:

2. Indicate a poorer prognosis and reduced efficacy of immunotherapy for endometrial cancer;
3. Assist in the molecular classification of endometrial cancer when there is a discrepancy between MMR-IHC and NGS-MSI results.
1.Nucleic acid extraction
2.Set up qPCR
3.Amplification
4.Data analysis
5.Report generation



 闽公网安备35021202000745
闽公网安备35021202000745